Chemo - and radiation therapy in non-small cell lung carcinoma
Patient S., 58 years old.
· Disease manifesto in December 2016 with fever up to 38 ° C, cough, shortness of breath with moderate physical exertion.
· Within 3 weeks he was treated independently.
· In January 2017, he turned to a therapist - a chest x-ray was performed. Suspected central cancer of the right lung.
· The patient's smoking experience is 28 packs / years.
CT OGP 06.01.2017. CT-picture of the intraluminal pathological soft component density (central cancer?) In the intermediate bronchus of the right lung with atelectasis of the lower lobe. Lymphadenopathy of the right root, quantitative lymphadenopathy of the mediastinum.
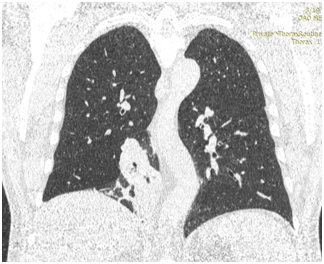
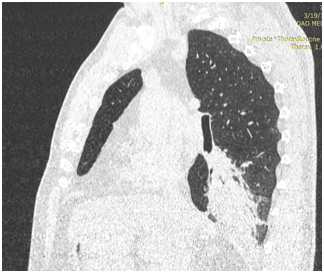
Bronchoscopy 01/11/2017.
Central cancer of the right lung.
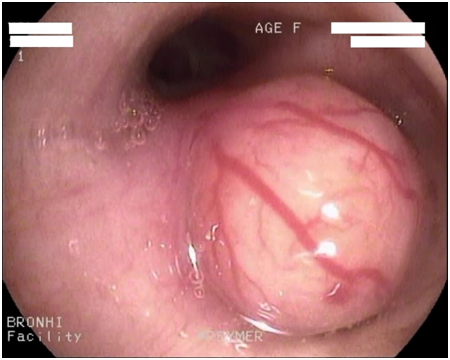
Histological report. Highly differentiated squamous cell carcinoma with keratinization (G1) throughout the entire thickness of the fragments.
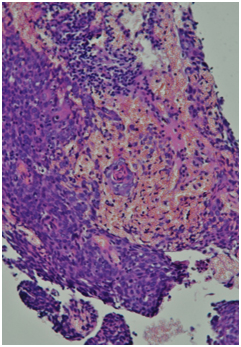
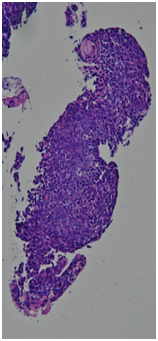
PET-CT from 01/12/2017. In the right lung, a soft tissue formation with a metabolic size of 30 × 24 mm with calcification in the structure SUVmax = 21.36 is determined, which overlaps the lumen of the intermediate bronchus on the right immediately after the level of the branch of the middle lobe bronchus with the formation of a picture of the "stump of the bronchus" - in the bifurcation lymph node up to 20 mm SUVmax = 4.77.
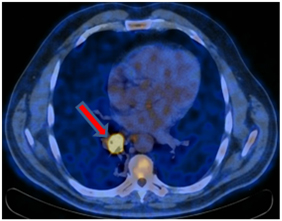
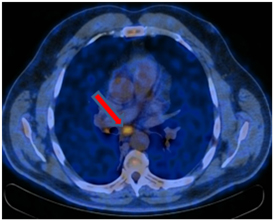
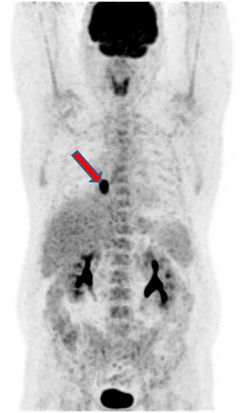
Staging. T1bN2M0 StIIIa.
Treatment options
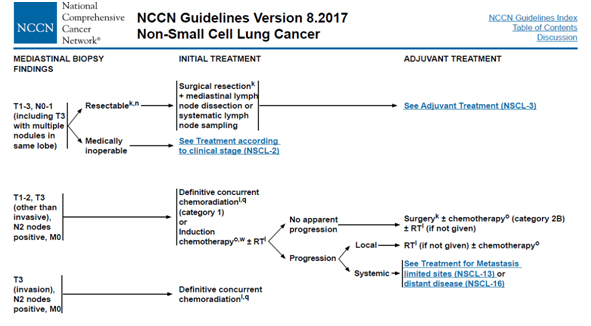
Oncological consultation 01/13/2017.
Chemoradiation therapy was recommended: for the main process in the right lung, mediastinal lymph nodes up to SOD 66 Gy for 33 fractions against the background of weekly chemotherapy: Paclitaxel 50 mg / m 2 + Carboplatin 2 AUC.
This treatment option was chosen due to the supposed low sensitivity of the tumor during morphological differentiation of G1 to induction chemotherapy and due to the fact that only pulmonectomy could be an option for surgical treatment due to the location of the tumor.
18.01.2017 - 03.03.2017. A radical course of radiation therapy for the primary focus in the right lung and the area of regional lymph drainage (PET - positive mediastinal lymph nodes) in a single dose of 2 Gy to a total dose of 66 Gy in 33 fractions. Duration of treatment is 6 weeks. There were 6 injections of Paclitaxel 50 mg / m 2 + Carboplatin 2 AUC weekly.
Tolerability of the treatment is relatively satisfactory. Added CSF from the 3rd week.
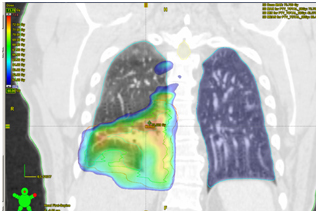
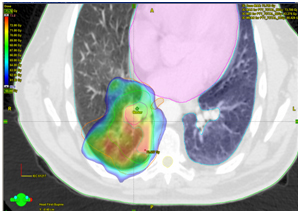
KT OGK dated 28.03.2017. Compared to the previous CT scan of 01/06/2017, there is a pronounced positive dynamics of changes due to the absence of formation in the lumen of the intermediate and lower lobe bronchi on the right, the absence of atelectasis of the lower lobe, as well as a moderate decrease in the number and size of lymph nodes in the mediastinum and the root of the right lung.
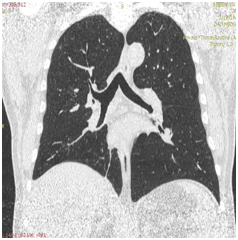
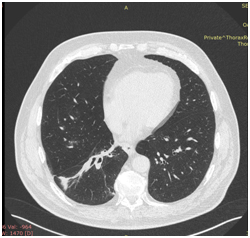
PET / CT from 31.05.2017. Positive dynamics is noted in the form of leveling the centrally located formation of the lower lobe of the right lung and mediastinal lymph node. Postradiation fibrosis, atelectasis of the lower lobe of the right lung. Moderately expressed right-sided hydrothorax. Increased metabolism in the cardiac esophagus is a post-radiation inflammatory process.
Clinically: moderate pain when swallowing solid food, shortness of breath on exertion, dry cough.
Anti-inflammatory treatment was carried out, a sparing diet was prescribed.
PET / CT 08/04/2017. At the time of the study, according to PET / CT with 18F-FDG, there were no signs of a pathological, metabolically active process caused by the underlying disease.
Postradiation fibrosis, atelectasis of the lower lobe of the right lung.
Moderately pronounced right-sided hydrothorax (increase in dynamics).
A metabolically active process in the cardiac esophagus was not identified at the time of the study.
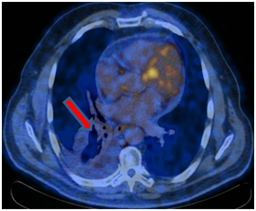
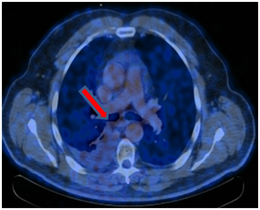
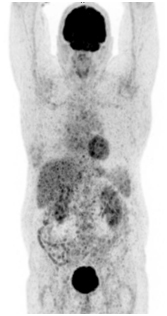
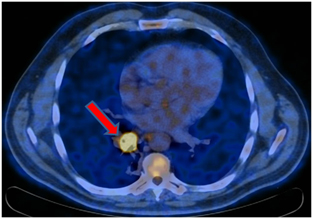
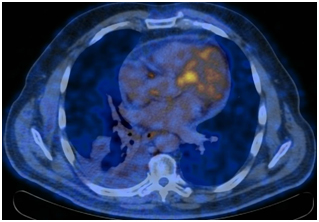
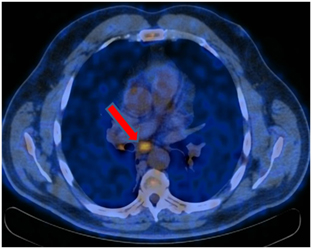
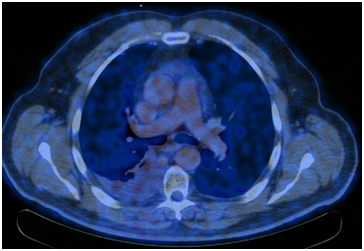
Conclusions.
Thus, a patient with stage IIIa central non-small cell right lung cancer underwent radical chemoradiation therapy with complete tumor regression.
The follow-up period after the end of therapy was 9 months: relapse-free course.
Clinically: the patient's condition is satisfactory, there are no signs of respiratory failure, the phenomena of post-radiation esophagitis are stopped.





