Gastroscopy
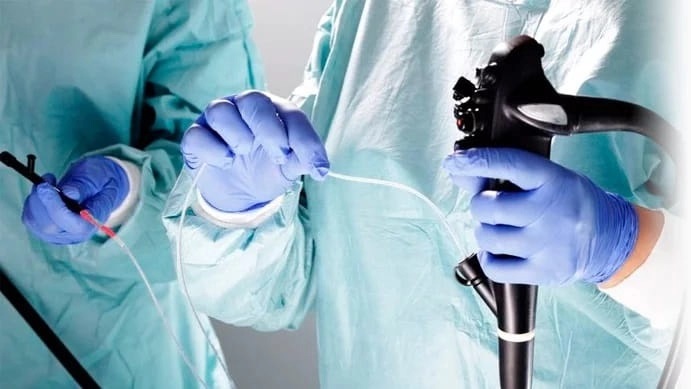 Gastroscopy remains the most common way of imaging the walls of the esophagus and stomach in the clinical setting. Doctors often use the full name of this procedure, esophagogastroduodenoscopy (EGD), when talking to patients. It appears under this name in medical manuals and other documents. Let's look at what patients should know about the procedure.
Gastroscopy remains the most common way of imaging the walls of the esophagus and stomach in the clinical setting. Doctors often use the full name of this procedure, esophagogastroduodenoscopy (EGD), when talking to patients. It appears under this name in medical manuals and other documents. Let's look at what patients should know about the procedure.
Indications
The list of abnormalities that require EGD is extensive. It includes any lesions of the upper digestive system and the stomach, despite their stage and ongoing therapy. The main indications for gastroscopy are regular stomach pain, frequent attacks of heartburn, intense belching, systematic vomiting and a feeling of heaviness and distention after meals.
Urgent or planned esophagogastroduodenoscopy is performed in the following cases:
- identification of signs of esophageal damage (stenoses, oesophagitis);
- search for a foreign body in the upper digestive system;
- diagnostic of gastric pathologies (gastritis, peptic ulcer, polyps, cancer);
- sampling of biological material for subsequent biopsies;
- stopping of internal bleeding on the background of peptic ulcer;
- spraying of medications on the areas of pathological processes;
- removal of polyps and other neoplasm.
Alternative scenarios for the use of EGD are determined by doctors based on the patient's condition and the clinical picture of the disease.
Contraindications
Gastroscopic diagnosis is considered by gastroenterologists to be a safe and simple procedure. An unsatisfactory condition of a person suffering from gastrointestinal pathology becomes a barrier to its carrying out. Absolute contraindications are:
- patients experiencing shock;
- shortness of breath and low blood oxygen levels;
- acute myocardial infarction;
- strokes of any kind;
- aortic aneurysm;
- coma in the absence of intubation;
- perforation of the esophagus and stomach.
The list of relative contraindications remains equally extensive. This list includes significant heart and lung failure, blood clotting disorders, recent heart attacks and strokes (less than six months since the acute stage of the pathologies was detected). CNS lesions are often considered by diagnosticians as a reason for not performing a gastroscopy. The inability of a person to independently follow his/her doctor's commands during the examination due to obesity or extreme exhaustion, enlargement of the thyroid gland, narrowing of the esophagus and significant deformations of the spine are among the list of relative contraindications for performing EGD. Before starting the diagnostic procedure, any patient should notify the doctor of a runny nose, enlarged lymph nodes in the neck and large diverticula in the esophagus.
Our doctors

General information
EGD is one of the diagnostic procedures aimed at detecting gastroenterological abnormalities. During the examination, a doctor obtains images of the tissues of the esophagus, stomach and part of the duodenum. The gastroscope used for this purpose is an elastic tube equipped with a camera, a lamp and micro-scissors for taking a biopsy sample. The sheath of the instrument protects the fiber optic strands from mechanical and chemical influences from the stomach content.
A gastroscope is part of a group of endoscopic instruments used by doctors in invasive procedures. Its use makes it possible to:
- assess the condition of the mucous membranes of the esophagus and stomach;
- detect pathological changes in the anatomy and function of the organs;
- detect ulcers, erosions and atrophies;
- diagnose malignant and benign neoplasms;
- carry out therapeutic procedures;
- collect biomaterials for tests.
Advantages of esophagogastroduodenoscopy
Advantages of EGD are:
- combination of diagnostic and therapeutic manipulation in one procedure;
- possibility of taking a biopsy sample for histological examination;
- high informative in diagnosing cancer in its early stages;
- no harmful effects on the patient's body.
When performing esophagogastroduodenoscopy, a doctor has the ability to stop internal bleeding, remove a foreign body from the gastrointestinal tract or carry out further tests if indicated.
Preparation
This diagnostic method is highly informative when all substances such as food debris and fluids drunk by the patient are completely removed from the organ under examination. For this reason, people undergoing EGD are advised not to eat any food 8-12 hours before their visit to the clinic. The only exception is an emergency gastroscopy, during which a gastric tube is emptied.
Patients should warn their doctors about undergoing an X-ray of the gastrointestinal tract using contrast agents. The minimum amount of time separating these tests must be at least 72 hours.
Before the gastroscope is placed in the patient's mouth, the doctor tells the patient how the procedure is conducted and warns about possible feelings of discomfort or heaviness. If indicated, the examination is performed under general anaesthesia (so-called "sleep gastroscopy"). Reasons for putting the patient to sleep are the length of the procedures to be performed or their painfulness.
Gastroscopy in the clinic
The order of actions of medical staff and people undergoing EGD is typical. The procedure consists of the following stages:
- the patient lies on the left side, with his/her knees pressed against his/her stomach and his/her back perpendicular to the couch;
- the oral cavity and pharynx are anaesthetised to prevent the development of a gag reflex or coughing attack;
- a mouthpiece is placed in the patient's mouth in order to prevent the teeth from closing and stop the gastroscope from moving;
- the doctor presses air into the patient's stomach to provide better visibility of the tissues;
- an endoscopic tube is inserted into the patient's oral cavity and gradually advanced into the lower parts of the digestive tract;
- if necessary, samples are taken for biopsy.
After all diagnostic and therapeutic procedures have been performed, the fibrescope is slowly removed from the stomach and esophagus to prevent tissue damage.
Taking biomaterials for biopsies
The fitting of the endoscope allows gastroenterologists to obtain material for subsequent histological examinations. Microscopic forceps provide an opportunity to capture tissue at the boundary of healthy and affected areas of the mucosa. The procedure involves taking several samples from each part of the stomach.
If signs of a malignant neoplasm are found, a chromoscopy is performed. Tissues are stained with an indicator dye that reacts with cancer cell antigens. This method allows the differential diagnosis to be made and the size of the tumors to be determined. This information will help doctors to develop a strategy for radical or conservative treatment.
Detection of Helicobacter pylori bacteria
Bipotage sampling from gastric tissue provides diagnostic laboratories with the ability to detect the extent of Helicobacter pylori presence in gastric tissue. This analysis includes:
- microscopy;
- immunohistochemistry;
- polymerase chain reaction;
- pH measurement, etc.
A swab taken from the surface of the stomach can be used as an additional measure. Its study helps to establish the extent of the mucosal lesion of the spiral bacterium and to develop an effective strategy for the medical treatment of the patient.




